A quarter-century ago, the United States successfully eliminated the measles virus. Known for its high contagion rates, occasional cases and outbreaks of measles are still anticipated.
As of February 28, 146 individuals in Texas, predominantly unvaccinated children, have been diagnosed with measles. The Texas Department of State Health Services reported that 20 of these cases required hospitalization. Tragically, one unvaccinated “school-aged child” passed away this week, marking the first measles-related death in the U.S. since 2015, as stated on February 26.
Health authorities in New Mexico also report nine additional cases in a nearby county.
Dr. Adam Ratner, a pediatric infectious disease specialist in New York City and author of *Booster Shots: The Urgent Lessons of Measles and the Uncertain Future of Children’s Health*, describes this situation as a significant outbreak. The CDC categorizes an outbreak as the occurrence of three or more related cases; in 2024, a total of 285 cases were confirmed in 31 states and Washington D.C.
For further insights into the measles virus outbreak, here’s what you should know.
What is the Recent History of Measles in the U.S.?
The most significant outbreak in recent U.S. history occurred in 2019, when nearly 1,300 people contracted the virus. According to the CDC, this surge nearly jeopardized the country’s measles elimination status, which is defined as no transmission of the virus for 12 consecutive months.
Dr. Peter Hotez, the dean of the National School of Tropical Medicine at Baylor College of Medicine in Houston, warns that the current situation is “just the tip of the iceberg,” predicting that case numbers may reach or even exceed those seen during previous outbreaks.
This increase is largely attributed to declining vaccination rates in both the U.S. and globally, leading to a fourfold spike in measles outbreaks from 2023 to 2024. Hotez adds, “I anticipate that 2025 is going to be a particularly challenging year for measles.”
What is Measles, and Who Typically Contracts It?
Measles is a highly infectious respiratory virus that primarily impacts children, although adults who have neither been infected nor vaccinated are also at risk, states Robert Bednarczyck, an epidemiologist and associate professor of global health at Emory University in Georgia.
While measles is often discussed in conjunction with mumps and rubella due to the MMR vaccine protecting against all three diseases, it is crucial to note that each illness is caused by a distinct virus.
How is Measles Transmitted?
The measles virus resides in the mucus of the nose and throat of infected individuals. When an infected person coughs, sneezes, or breathes, viral particles are propelled into the air, where they can remain viable for up to two hours. Dr. Hotez emphasizes that you don’t need to be in close proximity to an infected person to contract the virus, which is why measles is among the most contagious diseases known.
The CDC indicates that if someone with measles is present, up to 90% of unprotected individuals who inhale contaminated air or touch infected surfaces are likely to become ill. Unlike many other respiratory viruses, measles is not seasonal.
An individual with measles is contagious for about eight days, including four days prior to the onset of a rash and four days after. This presents a challenge, as noted by Ratner, since individuals can transmit the virus even before showing symptoms.
How Can I Tell If I Have Measles, and What Are the Symptoms?
Initial symptoms of measles may not be noticeable until one to two weeks post-exposure. During this time, you may experience a cough, runny nose, watery eyes, and high fever, according to the CDC. Initially, you might mistake these signs for flu, but within two to three days, you may notice tiny white spots inside your mouth, which Bednarczyck identifies as a telltale sign of measles.
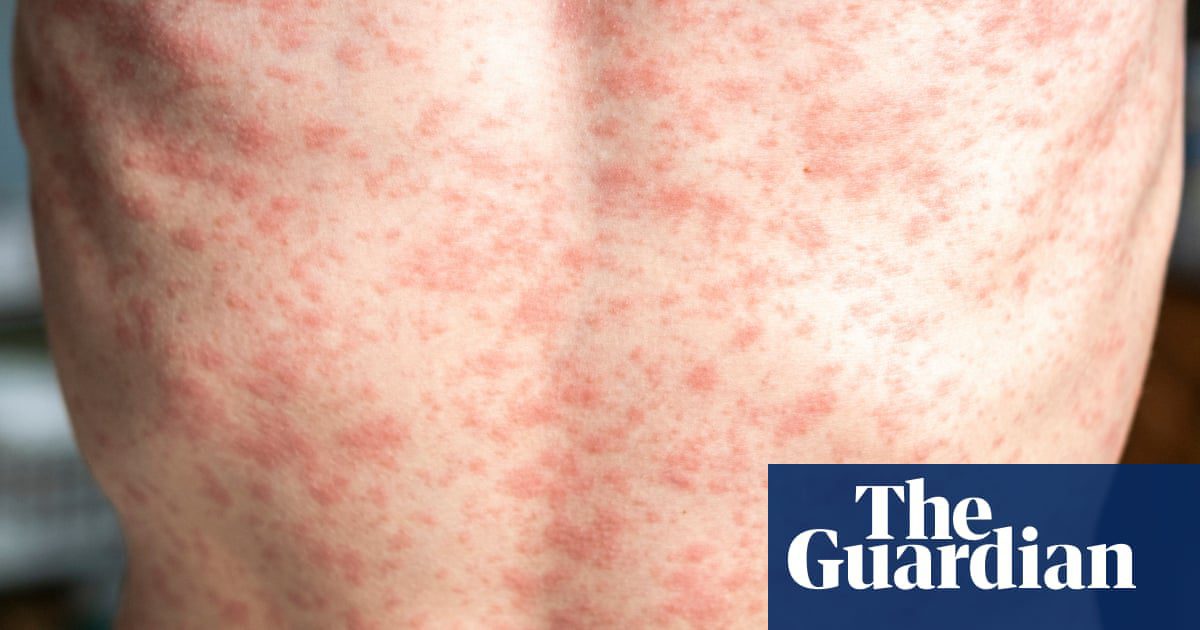
Within three to five days, the characteristic measles rash typically appears: red spots on the face that progressively spread to the neck, trunk, arms, legs, and feet, per the CDC. It’s noted that individuals with darker skin may exhibit small raised bumps in the same areas without color change. Although the rash appears severe, it generally does not cause itching.
In total, you may feel unwell for about one week, with the rash lasting five to six days. If you believe you or your child has measles, it’s advisable to call your healthcare provider before arriving to minimize exposure to others in the waiting area.
Do Most Individuals Recover from Measles?
The majority of individuals infected with measles recover without any long-lasting health issues, according to health specialists. However, complications can arise for a significant number of those infected, some of which can be quite severe.
after newsletter promotion
Ear infections are a common complication, affecting approximately one in every ten children who contract measles, according to the CDC. Pneumonia, which is the leading cause of measles-related deaths among children, occurs in as many as one in 20 cases. Encephalitis, a swelling of the brain that can result in deafness, seizures, or cognitive impairment, affects about one in every 1,000 children. Alarmingly, research indicates that one to three children in every 1,000 with measles may die from these complications.
Additionally, a rare but severe disease called subacute sclerosing panencephalitis may develop in a small number of individuals seven to ten years post-recovery from measles; this risk is greater for those infected before age two.
Those unvaccinated, young children under five, adults aged over 20, individuals with compromised immune systems, and pregnant women face heightened risks of measles-related complications, according to the CDC. However, it’s crucial to understand that anyone, regardless of health status, can suffer severe illness or even death from measles, stresses Ratner—particularly given that there are no effective treatments for the virus. Some hospitalized individuals may receive vitamin A, which could help mitigate adverse outcomes, but it is not a cure.
How Can Measles be Prevented?
As measles is an airborne virus, wearing face masks can provide additional protection against infection, experts advise. Nevertheless, vaccination remains the most effective preventive measure. Prior to the initiation of the U.S. measles vaccination program in 1963, approximately 3 to 4 million cases were reported annually, with 48,000 hospitalizations, 1,000 instances of encephalitis, and 400 to 500 deaths each year according to CDC statistics.
The vaccination process consists of two doses. The first is administered between 12 to 15 months of age and is about 93% effective, while the second dose, given between ages four and six, has an efficacy of approximately 97%. This means that around three out of every 100 vaccinated individuals may still contract measles after being exposed to the virus, according to CDC data.
Despite this, the vaccine significantly reduces the chance of developing severe illness and limits the potential spread to others, including those who cannot receive the vaccine due to their young age or weakened immune systems. Research also indicates that measles infection decreases the effectiveness of antibodies formed against other pathogens, leaving unvaccinated individuals susceptible.
Decades of research affirm that the measles vaccine is safe. A discredited 1998 study involving 12 children wrongly suggested a relationship between the MMR vaccine and autism; it has since been retracted for “scientific fraud.” Subsequent studies have firmly established that there is no causal relationship.
If you are exposed to measles and have not been vaccinated or received only one dose, it is possible to administer the measles vaccine within 72 hours to prevent infection or reduce the severity of the illness, according to Ratner. Additionally, young children who haven’t been vaccinated and individuals at high risk for severe disease might receive an antibody treatment known as immunoglobulin within six days of exposure, either intravenously or via injection in the arm.
Both measles infection and vaccination are believed to provide lifelong immunity, meaning you cannot contract measles twice. Nevertheless, if you are unvaccinated and have gone through measles, Ratner advises you to still receive the vaccine for protection against mumps and rubella.
The MMR vaccine contains a weakened form of the measles virus, producing a harmless infection that aids in building immunity. Therefore, some individuals should avoid the vaccine, according to the CDC, including pregnant women and those with compromised immune systems due to medical conditions or treatments.
Should I Be Concerned About Measles in the U.S.?
If you are vaccinated, the risk to you is minimal. Nonetheless, the CDC classifies measles as a public health concern in the U.S. The decline in children receiving their measles vaccinations worldwide, partly due to vaccine-related misinformation during the COVID-19 pandemic, could lead to an uptick in infections as unvaccinated travelers bring the virus back. “Our ability to control measles is a testament to vaccination and our preparedness, but we are on the verge of witnessing broader outbreaks,” Bednarczyck warns.
From the 2019-2020 school year to the 2023-2024 school year, vaccination rates among U.S. kindergarten students dropped from 95% to just below 93%. This decline is alarming, Ratner notes, as herd immunity—which prevents substantial outbreaks—requires around 95% vaccination coverage. In some states, the rates are even lower; for instance, in Idaho, the vaccination rate stands at 80%.









